A study on prevalence of shock among the paediatric age group in and around west Godavari district, Andhra Pradesh.
Incidence of shock among paediatric age group
Abstract
Introduction: Shock is one of the most common paediatric emergencies with significant mortality. Death is due associated complications and multisystem organ dysfunction. With these a study was conducted to find the prevalence of shock among the paediatric age group.
Materials and methods: Study was conducted in the department of paediatrics, ASRAM, Eluru, Andhra Pradesh, over a period of 18 months. Random sampling was considered in this study. Children aged 1 month to 12 years, admitted with clinical diagnosis of shock were included. Neonates and parents of those who didn’t submit the informed consent were excluded. Among the participants, shock was diagnosed by the standard protocol such blood smear examination, inflammatory markers, blood pressure. Chi square test was used to find the association between the variables and P < 0.05 was considered statistically significant.
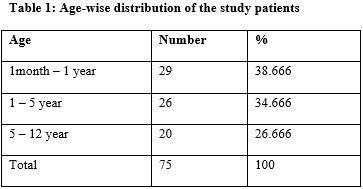
Results: Shock was diagnosed in 75 (7.96%), maximum (39%) were detected in 1 month to 1 year age group. Gender wise, 41 (54.6) members were male and 34 (45.3) members were female. The male female ratio was 1.2:1. Total 56 (74.6) were survivors and 19 (26.4%) were non survivors; statistically there was no significant difference.
Conclusion: Majority of shock cases were in cases were in the age group of >1month to 5 years age group.
Downloads
References
2. M Jayashree. Shock. Shock. IAP Textbook of Pediatrics. 6th edition. Jaypee brothers medical publishers. 1047 – 55.
3. David A, Turner, Ira M. Cheifetz. Shock. Nelson Textbook of Pediatrics. 20th edition. Elsevier Publishers 2016; 516 – 28.
4. Ruchi Sinha, Simon Nadel. Understanding shock. Pediatrics and child health. 2013; 23 (5): 187 – 93.
5. King EG, Chin WDN. Shock: an overview of pathophysiology and general treatment goals. Crit Care Clin 1985; 1: 547 – 56. PMID: 3870974.
6. Perkin RM, Anas NG. Nonsurgical contractility manipulation of the failing circulation. Clin Crit Care Med. 1986; 10: 229 – 34. doi: 10.1097/CCM.0000000000001379
7. Shamji Fm, Todd TRJ. Hypovolemic shock. Crit Care Clin 1985; 1: 609 – 14. PMID: 3916796
8. Ravikant M, H.K.G.Singh, Shrinivasreddy B. Clinical study of shock in children with special reference to prognostic determinant at teaching hospital, Bangalore. Med Innovatica.2015; 4 (1); 1 – 7.
9. Singh D, Chopra A, Pooni PA, Bhatia RC. A clinical profile of shock in children in Punjab, India. Indian Pediatr. 2006; 43(7): 619 – 23. PMID: 16891682.
10. El-Nawawy A, El-Kinany H, Hamdy El-Sayed M, Boshra N. Intravenous polyclonal immunoglobulin administration to sepsis syndrome patients: a prospective study in a pediatric intensive care unit. J Trop Pediatr. 2005; 51(5): 271 – 8. doi: 10.1093/tropej/fmi011. Epub 2005 May 25. PMID: 15917261.
11. Derek S.Wheeler, Rajit K. Basu. Pediatric shock: an overview. The Open Ped Med J. 2013; 7 (1): 2 – 9. DOI: 10.2174/1874309901307010002
12. Kana Ram Jat, UrmilaJhamb, Vinod K Gupta. Serum lactate levels as the predictor of outcome in pediatric septic shock. Ind J Of Crit Care Med.2011; 15 (2): 102 – 7. doi: 10.4103/0972-5229.83017.
13. de Freitas Aragão, de Fátima M, Albuquerque PM, Gonçalves de Mello MJ, Ximenes RA. Risk factors associated with death in children admitted to a paediatric intensive care unit. J Trop Pediatr. 2001; 47(2): 86 – 91. doi: 10.1093/tropej/47.2.86.
14. Chang P, Hsu HY, Chang MH, Lin FY. Shock in the pediatric emergency service: five years' experience. Acta Paediatr Taiwan. 1999; 40(1): 9 – 12. PMID: 10910577.
15. Kumar N, Thomas N, Singhal D, Puliyel JM, Sreenivas V. Triage score for severity of illness. Indian Pediatr. 2003; 40(3): 204 – 10. PMID: 12657751.
16. Hochman Hi, Grodin MA. Crone RK. Dehydration, diabetic ketoacidosis and shock in the Pediatric patient. Ped Clin North Am 1979; 26: 803 – 26. doi: 10.1016/s0031-3955(16)33786-5
17. Butt W. Septic shock. Pediatr Clin North Am. 2001; 48(3): 601 – 25. doi: 10.1016/s0031-3955(05)70330-8.
18. Khilnani P, Sarma D, Singh R, Uttam R, Rajdev S, Makkar A, Kaur J. Demographic profile and outcome analysis of a tertiary level pediatric intensive care unit. Indian J Pediatr. 2004; 71(7): 587 – 91. doi: 10.1007/BF02724117.
19. Watson RS, Carcillo JA, Linde-Zwirble WT, Clermont G, Lidicker J, Angus DC. The epidemiology of severe sepsis in children in the United States. Am J Respir Crit Care Med. 2003; 167(5): 695 – 701. doi: 10.1164/rccm.200207-682OC.
20. Carvalho PR, Feldens L, Seitz EE, Rocha TS, Soledade MA, Trotta EA. Prevalência das síndromes inflamatórias sistêmicas em uma unidade de tratamento intensivo pediátrica terciária [Prevalence of systemic inflammatory syndromes at a tertiary pediatric intensive care unit]. J Pediatr (Rio J). 2005; 81(2): 143 – 8. Portuguese. PMID: 15858676.
21. Ganjoo S, Ahmad K, Qureshi UA, Mir ZH. Clinical Epidemiology of SIRS and Sepsis in Newly Admitted Children. Indian J Pediatr. 2015; 82(8): 698 – 702. doi: 10.1007/s12098-014-1618-x.
Copyright (c) 2021 Author (s). Published by Siddharth Health Research and Social Welfare Society

This work is licensed under a Creative Commons Attribution 4.0 International License.


 OAI - Open Archives Initiative
OAI - Open Archives Initiative


